Our Medical Director, Dr James Mackay presented to some of the greatest minds in medicine about ‘Genetic testing for hereditary breast and ovarian cancer’ at the ESMED General Assembly.
This was a significant educational presentation in which he explains the clinical limitations of traditional genetic testing and the concept of introducing an innovative testing service into clinical care to reduce the risk of cancer developing.
We have summarised Dr Mackay’s presentation below, but the full presentation is available to watch at the end.
The traditional genetic testing process
Traditionally genetic testing has focused on only those who are at risk of developing cancer, such as breast and ovarian, due to their strong family history. This is illustrated in the diagram below.
Those who have been diagnosed with breast or ovarian cancer are represented in green, with the larger purple circle representing their relatives (who all have a slight risk of developing breast or ovarian cancer). The small red circle suggests those who are at higher risk of developing breast or ovarian cancer because of their strong family history.
Currently, only the small group of people, represented in red, are more commonly tested for cancer, leaving many relatives or even those without any family history uncertain about their level of risk.
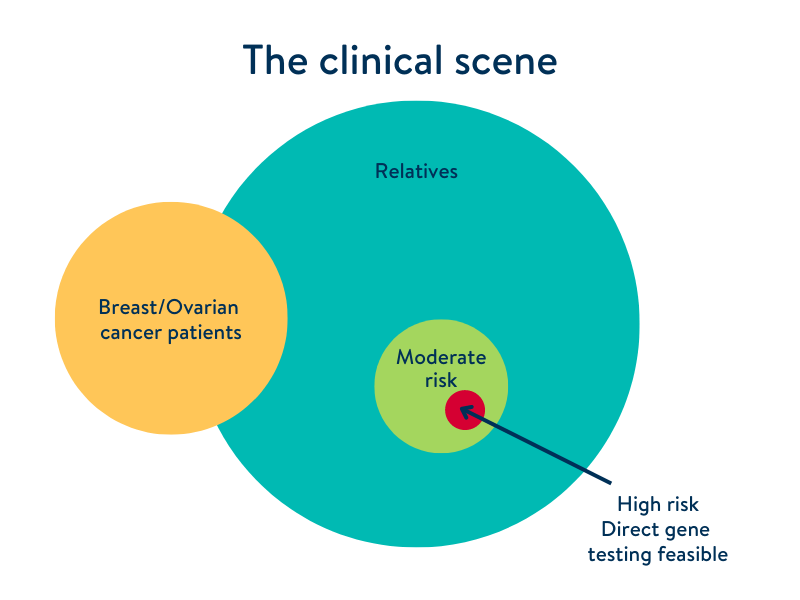
Traditional cancer risk testing practice in the UK
What does traditional genetic testing for breast or ovarian cancer involve?
Testing for breast and ovarian cancer involves analysing the complete sequence of a female’s BRCA1 and BRCA2 genes. These are made up of the letters C, G, A and T arranged in a long sequence of thousands of repetitive patterns.
The BRCA1 gene is made up of 100,000 letters arranged in sequence, and a faulty gene can be caused by a very subtle change in a single letter which can be found anywhere within the sequence.
Analysing the BRCA1 gene involves a two-step process:
Step 1: Identifying a fault within the family by taking a saliva sample from someone in the family who has or had ovarian or breast cancer.
Step 2: If a genetic fault is found, we can then test to find other similar genetic faults in other members of the family. If they don’t have the same genetic fault, we can assume that they have inherited a ‘good’ copy of the gene, but if the same faulty gene is found in several members of the family, things become a little clearer.
However, the issue with traditional cancer testing is that family history is used as a ‘guide’ to direct genetic testing, leaving individuals who have no, or distant family history of cancer with uncertainty.
The importance of weak gene panel testing
One solution to this is to analyse a wider gene panel which is a major step forward in genetic testing because it’s available to everyone regardless of their family history, and it looks at the entire gene panel to give a far more accurate result.
BRCA1 and 2 genetic tests are known as ‘strong gene panels’. Weak gene panel testing, however, analyses over 2,000 Single Nucleotide Polymorphisms (SNPs) and can identify when one single copy of a genetic sequence differs by a single base from the other copy. This result provides what is known as a polygenic risk score which gives a percentage risk of that person developing the cancer tested for against a woman of her age in the normal population.
The importance of weak gene panel testing is that the results only apply to the individual tested, with no implications for family members, and everyone who is tested gets a definitive personalised result on their risk of developing the cancer tested for.
Our mission is to make high-quality, low-cost cancer genetic testing available to as many people as possible. By persuading healthcare professionals to offer testing to their clients, irrespective of family history, it will allow everyone to be given accurate and understandable information about their own individual risk of developing common cancers.
Dr James Mackay’s presentation is available to watch in full here >>
To find out more about genetic risk testing services, email partners@everythinggeneticltd.co.uk or call +44 (0) 1270 623 179.



